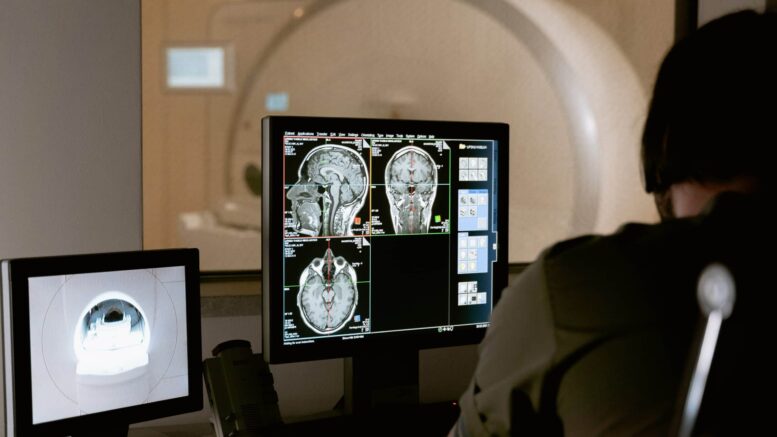
Teleradiology Services – Overview
What is teleradiology?
To clearly understand all terms, let’s define the word radiology first. Radiology is a special technique for taking internal images of the body. The prefix “tele” comes from Greek and means “far off,” or “afar”.
Thus, teleradiology refers to the practice of a radiologist interpreting study results while physically being away from the place where these images are generated. It is one of the most widespread branches of telemedicine.
Thousands of healthcare facilities all around the world rely on teleradiological services daily.
Why use teleradiology?
The primary benefit of this practice is cost reduction. It is really expensive to have a radiologist on-site. Daily costs are around 1,500$. Using teleradiology services enables healthcare facilities to pay per exam basis.
This approach provides huge savings to small clinics and hospitals with a minor amount of radiology patients.
The same is true for facilities requiring 24/7 access to radiologic services, as long as the majority of teleradiology providers have employees in different countries to maximize the time zone differences.
After-hours and weekend care costs are effectively cut this way.
Other advantages include improved quality of patient care by allowing access to subspecialists like musculoskeletal and pediatric radiologists, which would not be otherwise accessible. This is more beneficial to rural areas with a lack of qualified professionals.
Teleradiology services are used in ER. For example, in the case of orthopedic trauma images are sent to a subspecialist for better interpretation.
This allows faster communication and also helps to reduce time spent under ER care, which is quite costly.
Keep in mind, that teleradiology providers generally have less turnaround time (refers to the time it takes for a scan to be received, read, and a report returned to the facility) compared to on-site services.
History of Teleradiology
Teleradiology during its almost half a century history influenced the entire telemedicine industry. It always took advantage of the best technologies available at the time.
Dating back to the 1930s, doctors on the ocean liner Queen Mary used marine radio for purposes of a medical consultation with doctors onshore.
In the 1940s, the transmission of radiologic images via phone lines was a possible, but unreliable and time-consuming option.
During the 1960s and 1970s, with the improvement of the techniques of broadcast television, some hospitals began sending medical images about radiology, dermatology, and pathology.
Dr.Kenneth D.Bird an internist and pulmonary specialist set up an interactive television system between Boston’s Massachusetts General Hospital and Logan airport which could provide travelers with medical care. Similarly, closed-circuit televisions were installed in several other places.
These systems were limited by the technology of that time, transmission speed and image quality were low, on the other side the cost of such systems was extremely high. As a result, they were more exhibits than practical tools.
In the 1980s mail was used to send physical copies of radiological images to distant radiologists.
They would record a report and send it back to the original facility. So turnaround time was several days. To make matters worse, displaying digital copies on different manufacturers’ machines was very difficult.
To overcome this The National Electrical Manufacturers Association and American College of Radiology in 1983 joined forces and created an open standard for medical images to be digitally stored.
First and second versions: ACR/NEMA and ACR/NEMA V2.0. were not widely accepted by manufacturers.
The third version introduced in 1993 was called DICOM. Standard network support added to this edition made things easier and it became widespread.
Nighthawk, Radlinx, and vRad were pioneers in this field. Today hundreds of companies operate in the teleradiology market.
Downsides of Teleradiology
The most important concern is the quality of service. With so many players on the market, it is hard to check the qualification of the radiologist on the other side.
This has already caused problems for European hospitals that tried to cut costs by outsourcing diagnosis and using Asian platforms for teleradiology services.
Apart from that, teleradiologists cannot perform any additional tests and need to rely on information from on-site caregivers. That can cause miscommunications.
Another drawback is inefficient international regulatory frameworks, which makes practicing cross-border teleradiology services too complicated, as they include foreign specialists, that need to be accredited in both countries.
Summary
Teleradiology already offers numerous benefits to small hospitals, rural areas, and 24/7 service providers. New technologies will contribute to the faster and more reliable interpretation of images.
Perhaps, the most impressive developing aspect is the use of AI, which will soon autonomously recognize emergency conditions like pulmonary embolism and alert the radiologist, to reduce the probability of human error to zero.
According to statistics, the need for imaging procedures is rising by 15% annually.
If we compare that to an annual 2% increase in the radiologist population, it will be clear that the teleradiology market has a space to grow and flourish.
References
https://www.ncbi.nlm.nih.gov/pmc/articles/
https://www.statrad.com/teleradiology-services/
https://en.wikipedia.org/wiki/

As a nutritionist, I research, find and experiment with recipes, natural diets and meal plans for weight loss, bodybuilding, and detoxing.